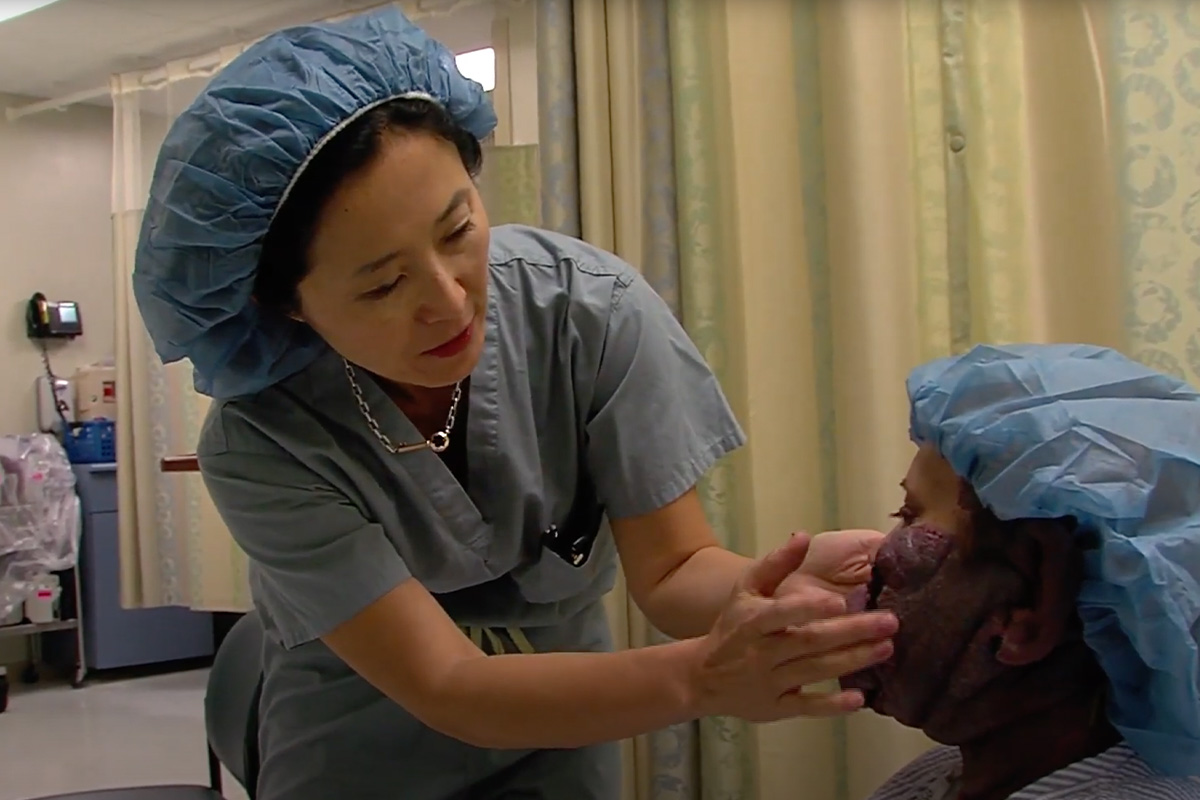
Port wine stains appear as reddish or purplish discolorations on the skin and may thicken or develop nodules over time. Led by Dr. Waner and Dr. O, the Vascular Birthmark Institute specializes in diagnosing and treating port wine stains in NYC to ensure the best aesthetic and functional outcomes for all ages.
What Are Port Wine Stains?
Port wine stains are vascular malformations caused by dilated capillaries just beneath the skin, resulting in red to purple discoloration that can darken or thicken with age. These lesions are usually present at birth and often affect one side of the body in a segmental pattern. While typically harmless, port wine stains can sometimes be associated with syndromes like Sturge-Weber Syndrome—a neurological condition involving skin, eye, and brain abnormalities that can cause seizures or vision loss in rare cases—and may require evaluation and management.

Signs & Symptoms of Port Wine Stains:
- Flat, pink, red, or purple skin discoloration at birth
- Commonly affects the face, neck, arms, or legs
- Color may deepen with age, emotion, heat, or physical activity
- Lesion may form nodules (cobblestones) from the mid-20s to the 60s (NOT inevitable)
- Possible soft tissue overgrowth in the affected area
- Risk of associated syndromes, such as Sturge-Weber Syndrome (NOT inevitable)
- May involve the eye, potentially leading to vision issues (NOT inevitable)
- Typically confined to one side or segment of the body
Treatments for Port Wine Stains in NYC
At the Vascular Birthmark Institute, we specialize in treating port wine stains in NYC, beginning with a comprehensive evaluation to assess the type, depth, and extent of the lesion. Our team, led by Dr. Waner and Dr. O, develops a personalized treatment plan based on your skin type, lesion characteristics, age, and any associated soft tissue or eye involvement. While not all port wine stains require treatment, we may recommend several options to improve both appearance and quality of life.
No Treatment
In some cases, especially when the lesion is light, stable, and not located on a cosmetically or functionally sensitive area, you may choose not to undergo treatment. Port wine stains are benign and do not always require medical intervention. However, it’s important to monitor for any changes over time, including thickening, nodule development, or signs of tissue overgrowth. We’ll help you understand the long-term considerations so you can make an informed decision.

Laser Therapy
Laser treatment is the most effective and commonly used approach for lightening port wine stains. We typically use pulsed dye laser (PDL) technology, which targets the dilated capillaries beneath the skin. The laser emits a burst of concentrated light absorbed by the red pigment in the blood, causing the abnormal vessels to collapse without damaging the surrounding tissue. Over time and with multiple sessions, this can significantly lighten the stain. In some cases, deeper or more resistant lesions may require advanced laser systems.
Cosmetic Camouflage
If you prefer not to pursue laser treatment or are in between sessions, high-quality medical-grade cosmetic camouflage can help conceal the discoloration. These products are designed to match your skin tone and remain in place throughout the day. Our specialists can help you choose the right cosmetic formulations and teach you application techniques for natural-looking coverage. While camouflage doesn’t treat the underlying condition, it can improve confidence and comfort in social settings, especially for facial lesions.
Schedule Your Consultation
Vascular Birthmark Institute is a leading center for the diagnosis and treatment of vascular birthmarks and malformations. With decades of experience, our team, led by Dr. Waner and Dr. O, offers compassionate care for port wine stains in NYC using the most advanced medical technologies. Whether you’re seeking treatment for a new diagnosis or exploring options for a longstanding port wine stain, we’re here to help you achieve the best possible outcome. Schedule your consultation today.
Contact Vascular Birthmark Institute Today